Editor's note: This column has been updated for clarity.
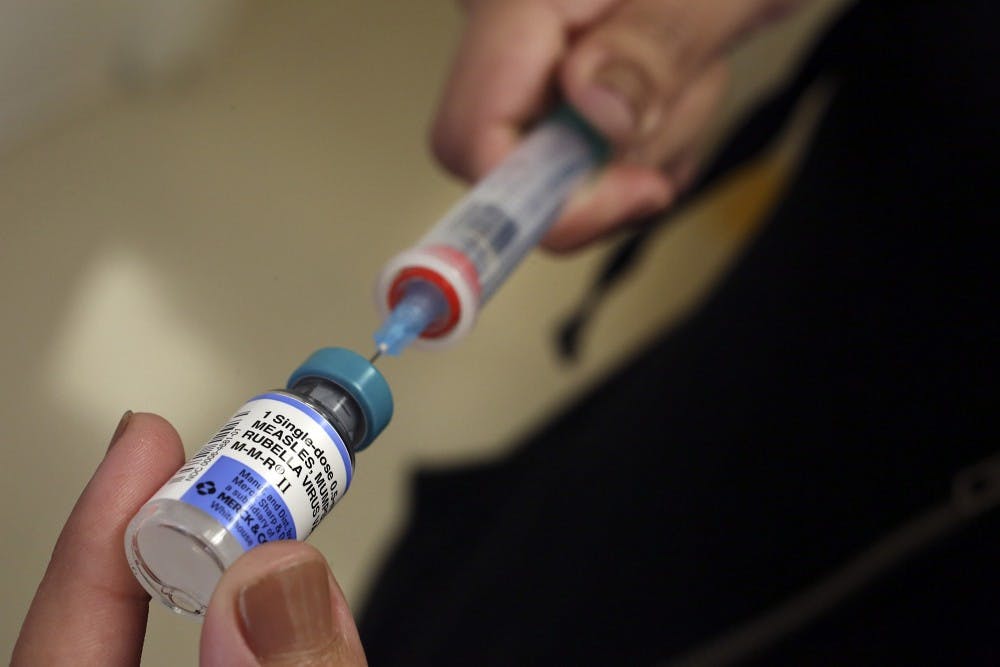
A measles outbreak in Washington has led Gov. Jay Inslee to declare a state of emergency. In Clark County, 41 out of 49 measles cases were not vaccinated against the disease.
This is not an isolated case. Outbreaks in New York state and New York City have also been reported in 2019.
Of course, not everyone who goes unvaccinated does so by choice. Some individuals have serious allergies to vaccinations or diseases that compromise their immune systems. Nonetheless, these outbreaks reveal that resistance to vaccination is a major public health issue in the United States and worldwide.
The World Health Organization declared that addressing vaccine hesitancy, defined as “the delay in acceptance or refusal of vaccines despite availability of vaccination services,” is one of ten threats to global health in 2019.
An analysis of 2015 to 2017 data from the WHO and the United Nations International Children’s Emergency Fund found that the top three reasons for vaccine hesitancy were risk-benefit concerns, parental lack of knowledge on the benefits of vaccination and cultural or religious beliefs.
Understandably, vaccine hesitancy frustrates a lot of health professionals and people.
When I was in Washington, D.C., for a Centers for Disease Control and Prevention conference last year, I remember sitting in a coffee shop while health professionals lamented the story of a woman who vaccinated her first child but not her second or third. How incredibly unfair to the children, they said.
When I’ve shadowed physicians, pediatricians have commented on the difficulties of communicating with parents who are opposed to vaccinating their children. Some providers have told me that they simply turn the parents away if they don’t change their mind.
Clearly, these are not the best options. Although there’s lots of judgement against those who choose not to vaccinate, one thing I don’t see addressed as often is what interventions can change their minds.
A 2015 systematic review found the most effective interventions for reducing vaccine hesitancy and increasing vaccination knowledge had multiple components and engaged people in dialogue. In other words, the research suggests that talking to people, more than posters or cash incentives, can change their mind on vaccination.
Indiana University currently allows for students to obtain religious exemptions for required immunizations. When I contacted the Office of the Registrar, I was unable to find how many students claim religious exemption from immunizations.
However, a 2013 systematic review found that introducing personal belief exemption categories often leads to increases in nonmedical exemption rates, but acknowledged a need for better quality studies to confirm this finding. Removing the category altogether in Indiana schools, along with improving vaccination and education programs, could prevent outbreaks like the one in Washington from happening in Indiana.
Pointing fingers is not going to help clarify misconceptions on vaccination. Changes in school policies on immunizations and evidence-based interventions will.